All published articles of this journal are available on ScienceDirect.
Stroke: Bowel Dysfunction in Patients Admitted for Rehabilitation§
Abstract
Aim :
to assess the prevalence of diminished frequency of bowel movements, lumpy or hard stools, intestinal constipation, straining, incomplete evacuation, incontinence (bowel dysfunctions) in patients with brain injury resulting from cerebrovascular accident, either self-reported or reported by their caregivers; to describe the type and frequency of such dysfunctions; and the prevalence of laxative use both before and after stroke.
Method :
cross-sectional study with 98 hospitalized patients admitted for rehabilitation between December 2009 and May 2010.
Results :
the prevalence of bowel dysfunctions before stroke was 23.96% whereas after the lesion it was 55.21% (p<0.0001). As reported by patients/caregivers, the chances of developing bowel dysfunctions increase sevenfold after stroke, 95% CI (2.44-24.26). The most frequent dysfunctions before stroke were intestinal constipation (73.91%) and diminished frequency of bowel movements (17.39%). After stroke, constipation remains to be the most frequent dysfunction reported (50%), followed by diminished frequency of bowel movements (26.79%), incomplete evacuation (12.50%), and lack of privacy (5.36%). The use of laxatives was 19,15% after the lesion, but not statisticaly significant (p=0.0736).
Conclusion :
Bowel dysfunctions increases significantly after stroke. Therefore, further studies are needed to better understand and characterize such dysfunctions, which are scarcely described in the literature.
INTRODUCTION
Cerebrovascular accident (CVA) or stroke is considered to be the second leading cause of death in the world [1]. In Brazil, according to a survey conducted by the Ministry of Health in which data collected over a period of 16 years (between 1990 and 2006) were analyzed, stroke is the leading cause of death amongst cerebrovascular diseases and the seventh cause of hospitalizations [2]. The gastrointestinal tract can be affected after a stroke, with dysphagia and alterations in the intestinal rhythm being the most common manifestations [3]. Motor, cognitive, and communication alterations may ensue and thus impair the dynamics for defecation to occur at a socially acceptable place and time [4]. Nevertheless, the specific changes that take place in the gastrointestinal tract after a stroke, which is responsible for causing such alterations, still need further investigation [5].
The main alterations in intestinal rhythm are intestinal constipation and fecal incontinence, whose prevalence varies depending on the definitions used in the studies, staging of the lesion and type of study. The prevalence of intestinal constipation varies between 22.9 and 60% [3, 6-11], whereas that of fecal incontinence oscillates between 31 and 40% in the two weeks following stroke [12], and between 9 and 15% in its chronic phase [5].
The definition of intestinal constipation is not a simple one. It can be influenced by cultural factors, therefore one needs to take into consideration both subjective and objective aspects when diagnosing it [13]. Intestinal constipation may thus be defined as the elimination of hard and dry stools with a frequency lower than three bowel movements a week; unsatisfactory or unsuccessful evacuation; or as the general assessment of any difficulty completing the act of defecation, such as need for straining, manual handlings, or excessive time spent on the toilet [13, 14]. According to the most common definition, anyone showing two or more of those symptoms can be considered constipated [13].
Fecal incontinence is a condition that restricts one’s social interactions and can be characterized as the incapacity for keeping one’s physiological control at an appropriate time and place. It is estimated that between 0.5% and 5% of the general population have fecal incontinence [15, 16].
Under the neurological rehabilitation program kept by Hospital SARAH-Brasília, which integrates the SARAH Network of Rehabilitation Hospitals and provides free care to the Brazilian population, we observed reports provided both by patients and their caregivers describing difficulties related to evacuation and expectations of improved bowel function. When facing such problems, an interdisciplinary team must also advise patients and caregivers on measures that can alleviate symptoms and promote bowel retraining. Still, the literature on programs able to provide for better care of this specific population is scarce. A better understanding of these symptoms, as self-reported by patients and their caregivers, will allow for establishing bowel retraining strategies that have a positive impact on the patient’s expectations.
The current study thus aimed to assess the prevalence of diminished frequency of bowel movements, lumpy or hard stools, intestinal constipation, straining, incomplete evacuation, incontinence (bowel dysfunctions) before and after stroke as self-reported by patients (or reported by their caregivers) with brain injury resulting from it; to describe the type and frequency of such disorders, and the prevalence of laxatives use both before and after stroke.
METHOD
The current cross-sectional, descriptive survey study was conducted between December 2009 and May 2010 at a neurological rehabilitation unit at SARAH Network of Rehabilitation Hospitals.
Sample and Setting
To be included in the study were patients of both gender with brain injury resulting from hemorrhagic and ischemic stroke, regardless of time past since injury and extent of cognitive impairment and language alteration. Impairment were evaluated by administering a Brazilian version of the Mini-Mental State Examination test [17]. For the examination, interviews were conducted directly with the patients who showed no signs of cognitive and/or language alterations. For those who had such alterations, the interviews were carried out with their caregivers, provided that they were familiarized with the patients' lifestyle habits and bowel function characteristics.
We excluded patients from those who: a) did not confirm vascular brain injury by imaging tests (computerized tomography or magnetic resonance image); b) besides vascular brain lesion had spinal cord injury of any type; c) had caregivers who were not familiarized with their lifestyle habit and bowel function characteristics; or d) planned to be readmitted to hospital over the period of data collection.
During the period of data collection, 120 patients were hospitalized, among whom 98 met inclusion criteria and were thus evaluated. 22 patients were excluded, 5 of whom opted not to participate in the study, and another 2 who did not provide all of the necessary information. The remainder did not meet inclusion criteria.
Data Collection Procedure
Data were collected by means of a structured interview that comprehended socio-demographic information, the presence of bowel dysfunctions, type of dysfunctions (as perceived by the patient/caregiver), and use of laxatives. The patients were surveyed regarding their condition both before and after stroke.
The semi-structured interview was used during the first thirty days of data collection. This instrument was applied at admission or up to a maximum of 72 hours from admission, by the researcher and two other specifically trained nurses.
The institution’s Research Ethics Committee previously approved the project, letter of approval number 518. Written informed consent was obtained from participants who were not cognitive impairment and can sign up the form, otherwise the consent were obtained of their guardians.
Statistical Analysis of Data
The odds ratio, point estimation and 95% confidence interval, for presenting bowel dysfunctions as reported by patients or their caregivers before and after stroke was calculated
McNemar’s test was used for assessing the percentage of patients having defecation disorders and using laxatives before and after stroke.
The level of statistical significance was set at p < 0.05. SAS 9.2® for Windows® was used for statistical analyses.
RESULTS
Fourty nine (50%) out of 98 patients were women. Regardless of gender, the mean age was 58.13 years with a standard deviation of 12.64, age varying between 28 and 87 years. The patients were predominantly white (56.12%), illiterate/primary school (45.91%), and married (63.26%). Regarding the lesion characteristics, the cerebrovascular accidents were predominantly ischemic (88.77%) and involved the left side of the brain; with an average time of 1101.42 days since the lesion and standard deviation of 1296.20.
By asking patients/caregivers if they believed to have any difficulty passing stool before and after stroke, and what those difficulties could be, it was verified that the chances of having bowel dysfunctions had increased sevenfold after stroke as compared before it. Twenty four (23.96%) of patients reported having bowel dysfunctions before stroke, whereas after the lesion 56 (55.21%) patients reported having such difficulties - statistically significant difference (p < 0.0001) (Fig. 1).
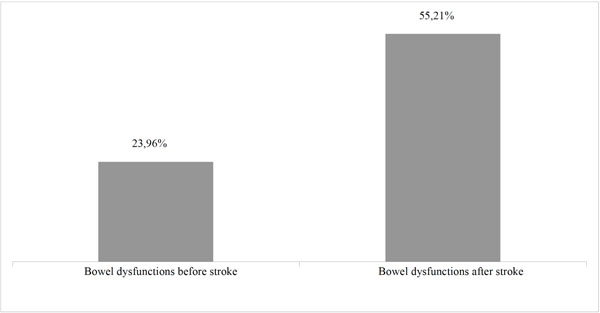
Frequency of bowel dysfunctions reports in patients before and after stroke (n= 98) (p < 0.0001).
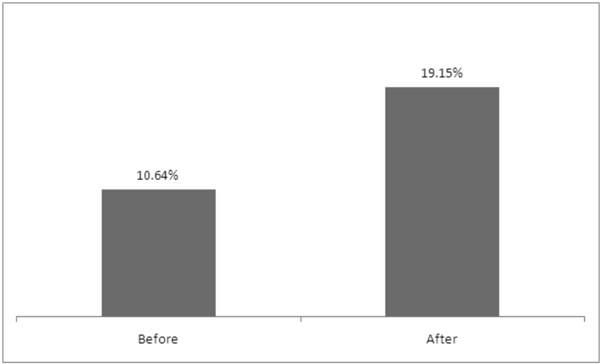
Frequency of laxative use before and after stroke (p=0.0736).
The most frequent dysfunctions before stroke were intestinal constipation, reported by 17 (73.91%) patients, and diminished frequency of bowel movements, with 4 (17.39%) such cases. After stroke, constipation remained the most frequently reported dysfunctions, with 28 (50%) cases. Nonetheless, other dysfunctions were reported, with the decrease in bowel movement frequency being the second most common dysfunction with 15 (26.79%) cases. Following those, we have incomplete evacuation with 7 (12.50%) cases, and lack of privacy with 3 (5.36%) cases (Table 1).
Complaint distribution by bowel dysfunctions reported by patients/caregivers before (n= 23) and after (n=56) stroke.
| Bowel Dysfunctions | Before | After |
|---|---|---|
| n (%) | n (%) | |
| Diminished frequency of bowel movements | 4 (17.39) | 15 (26.79) |
| Lumpy or hard stools | 1 (4.35) | 1 (1.79) |
| Constipation | 17 (73.91) | 28 (50.00) |
| Straining | - | 1 (1.79) |
| Incomplete evacuation | - | 7 (12.50) |
| Incontinence | - | 1 (1.79) |
| Lack of privacy | 1 (4.35) | 3 (5.36) |
| Total | 23 (100) | 56 (100) |
In this sample, it is possible to observe the frequency of patients that used laxative before and after stroke. A comparative analysis was carried out for this information and the proportion of individuals using laxatives before stroke (10.64%) is not statistically different (p=0.0736) from the one after stroke (19.15%) (Fig. 2).
DISCUSSION
The current study aimed to identify the frequency and type of bowel dysfunctions before and after stroke as perceived/reported by patients and their caregivers (for those patients having cognitive and language alterations), and the prevalence of laxative use in this population.
According to the results described in the previous section and as reported by patients or their caregivers, there was a significant increase in bowel dysfunctions after stroke. We could not identify in the literature studies that evaluated bowel dysfunctions as self-reported by patients with brain injuries resulting from stroke or as reported by their caregivers. However, we believe it is important to know such perceptions/reports for clinical practice. It can be observed in this study that some patients and caregivers do not define their bowel problem as specifically being intestinal constipation or fecal incontinence. There exist other complaints of discomfort that cannot be identified by the rehabilitation team.
Intestinal constipation is the most frequently reported dysfunctions, corroborated by findings in the literature. There are studies based on different definitions and investigation moments showing that the prevalence of this syndrome in the population with brain injury resulting from stroke varied between 22.9 and 60% [3, 6-11, 18]: in certain cases, the prevalence was investigated in patients whose injury was either more acute or more recent [6, 8, 11], whereas in others, chronic patients were evaluated [3, 10, 18], which may constitute the main factor for the differences in prevalence. For the current study, we looked in the reports from patients or their caregivers for dysfunctions referred to as being most disturbing. Besides constipation and fecal incontinence, we sought to identify other complaints of discomfort impairing patients’ quality of life.
Besides the frequently reported cases of constipation, we observed that, after stroke, patients also complained about a diminished frequency of bowel movements, incomplete evacuation, ad lack of privacy. In a study with this same population using Rome criteria for the definition of intestinal symptoms, the authors identified 55 (61%) patients with altered bowel function [3]. Among these, 33 (37%) reported decreased frequency; 30 (33%), straining or pain during defecation; 29 (32.2%), elimination of hardened stools; 21 (23.3%), incomplete evacuation sensation [3]. In our study, many of the patients referred to their most disturbing dysfunction, since they were instructed to spontaneously report their problems and were not given options from which to choose as occurred in the aforementioned study. Its authors describe the main symptoms according to known criteria, which are used in most studies to define functional intestinal constipation. Nevertheless, there exist divergences as to using such criteria for evaluating neurological patients.
The population evaluated in our study may thus have reported solely their most disturbing dysfunction, which could have led to the occultation of other relevant symptoms for better defining a condition that involves intestinal constipation and fecal incontinence. Only one single patient reported fecal incontinence, whereas its prevalence was 18% in another study [18] involving the analysis of the medical records of 138 patients, in which intestinal incontinence was investigated in association with the need for using diapers and patients not requesting to defecate. In the current study, this data may have been underestimated.
When reporting their bowel dysfunctions, three patients referred to lack of privacy. The literature suggests that this problem may occur after stroke and if privacy is not restored to the patient, he or she may become constipated [19].
After stroke, several aspect of the patient’s personal life may be affected, which can thus contribute to increased risk factors for developing bowel disorders, such as reduced physical mobility; fluid intake, since the patient may have difficulty swallowing, reaching for liquids or decreasing fluid intake in an attempt to control urinary incontinence; reduced fiber intake due to difficulty swallowing; dependence on others to use the toilet; reduced or absent urge to defecate; cognitive impairment; and use of medications that can affect bowel function [19].
As to physiological aspects that can be impaired, lesions affecting the pontine defecation center can interrupt defecation’s sequence of sympathetic and parasympathetic components, which may predispose fecal impaction and hinder the coordination of the peristaltic wave, relaxation of the pelvic floor and external anal sphincter. Such lesions may also impair rectal sensation, thus leading to an increase in rectal volume capacity, and resulting in fecal impaction in patients with a sensory loss in this region [20].
One factor leading to the high frequency of bowel dysfunctions is the frequency of laxative use. Among patients with bowel symptoms, 19.15% used some kind of laxative. In another study, the authors identified a prevalence of 24.4% [3]. It is noteworthy that the laxatives most commonly used by patients are the stimulant ones, the cheapest and best known. Their use, however, needs to be discontinued while patients are participating in a bowel retraining program [21]. An early identification of the use of laxatives as soon as a patient’s admission at the rehabilitation program may enhance the definition of his or her bowel retraining program. In our experience, patients using laxatives on a long-term basis normally do not respond to dietary and behavioral measures alone. They need to start the bowel retraining program with aid of some associated pharmacological measure, thus increasing their chances for effectiveness in the program [11].
The current study faced some limitations: 1) it was not a population study, which constitutes a selection bias, considering that the characteristics may differ from those of a general hospital; 2) in the case of patients with cognitive and language alterations, we needed to include information from their caregivers, which may hinder data quality; nevertheless, we tried to minimize this bias by including caregivers who knew the patients. On the other hand, one factor contributing to the veracity of information was the fact that the caregivers were usually the patients’ next of kin; 3) information regarding alterations prior to the injury may be biased as to its standardization/collection [22]; 4) and, lastly, the fact that no specific bowel disorders were listed, which might have helped patients' recollection; however, had we used such a list, we would not have been able to address the study's main goal: to identify, as perceived by patients/caregivers, the defecation disorders after stroke.
Understanding bowel dysfunction, as self-reported by patients and their caregivers, may contribute to the development of bowel retraining programs that can have a positive impact on these complaints. In future studies, we could investigate a treatment based on dietary and behavioral measures and assess their impact on patients’ complaints, as well as that of bowel dysfunction on the patients’ quality of life and the risk factors associated with bowel dysfunctions.
CONCLUSION
In the current study, we could verify that the number of defecation disorders significantly increased after the occurrence of a vascular brain injury as reported by patients or their caregivers, with the main complaints being constipation, decreased bowel movement frequency, incomplete evacuation and lack of privacy.
Early identification of the group of patients who frequently use laxatives is necessary to ensure that the bowel retraining program can start appropriately, achieve greater compliance with the dietary and behavioral measures and, thus, better performance.
Reports of bowel dysfunctions following stroke, which can impair the quality of life of patients and their caregivers, are common. Consequently, further studies in this field aiming to better understand such reports and contribute with additional knowledge to this poorly clinical area are necessary and expected to have a positive impact on proposals for treatment.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Acknowledgment is given to Eduardo Freitas da Silva, professor at the Department of Statistics at University of Brasília (UnB), for statistical advising and analysis.


