All published articles of this journal are available on ScienceDirect.
Reflections on the Centenary of Sir William Osler: Science and Humanity are One, for Nursing and Medicine
Abstract
Sir William Osler (1849-1991) was Regius Professor of Medicine at the University of Oxford in the UK and a founding professor at Johns Hopkins Hospital. The centenary of Osler’s death is a time for recognition in nursing, as well as medicine, of a pioneering and highly influential Oxford physician on both sides of the Atlantic, an influence that extended to nursing from the UK to the USA.
This letter captures reflections and discussion on contemporary nursing issues from an Osler Seminar Series, held at the University of Oxford in 2019 to mark the Centenary of Sir William Osler’s death, focusing on his thinking and influence related to nursing.
This extended letter illuminates issues on themes of science and humanity within a clinical and educational context, exploring a range of key contemporary nursing issues. These include the significance of interpersonal relations as they relate to care attitude and care technology; the therapeutic influence of the nurse; nursing education and clinical-academic development; the value of a life world perspective on nursing and wellbeing; and practice development within the context of person-centred workplace cultures. These issues are contextualised with examples from practice and include some from nursing developments and those illustrated in part by the clinical speciality of dermatological care.
The letter concludes by considering the significance of the nursing service to promoting access to quality health care in the twenty-first century and its relevance to recognising the nursing contribution to universal health care through the WHO International Year(s) of the Nurse and Midwife in 2020-21.
1. INTRODUCTION
The centenary of Sir William Osler’s death is a time for celebration in nursing as well as medicine [1] of a pioneering and highly influential physician on both sides of the Atlantic. At his Oxford home, where the Osler McGovern Centre is sited and owned by Green-Templeton College at the University of Oxford, we conducted five seminars on the theme For Health and Wellbeing, Science and Humanity are one. It was held in memory of his final lecture in 1919, The Old Humanities and the New Science [2]. It is a theme supported by his admirer, the American philanthropist, John McGovern, from whom in each seminar we quoted: “ The practice of medicine requires knowledge and skill, frequently labelled as the science andart of medicine, yet, knowledge and skill are incomplete without the steadying infrastructure of humanistic values and objectives” [3]. In Cambridge in 1959, a Rede Lecture by C.P. Snow [4] suggested that science and the humanities were mostly separated, and scientists and humanists at the high table could not converse. In this report on the centenary Osler seminar devoted to the nursing profession, we discuss a range of relevant issues with a focus on contemporary nursing but refer briefly to some of the other seminars concerning healthcare worldwide. We provide some historical context regarding Osler’s thinking relevant to nursing practice and their contemporary resonance, including the relevance to specific clinical examples, including ‘the case of dermatology' and clinical-academic nursing developments within Oxford and further afield.
Professor Terence Ryan, who developed the Osler seminar series, argued for the need to reinterpret the theme of For Health and Wellbeing, Science and Humanity are one, as the necessity to understand, apply and integrate care technology with care attitude when exploring the therapeutic dimension of medicine, and indeed that of nursing. Osler believed that a key therapeutic influence arose from the provision of friendship within practise. A century later. Oxford psychologist Professor Robin Dunbar’s study of the amygdala concluded that “Friendship is the single most important factor influencing our health, wellbeing and happiness.” [5]. Here we will discuss this notion within the wider context of Osler’ ideas, examine their relevance to contemporary care in the twenty-first century.
1.1. Care Attitude
Osler's ideas have longstanding relevance to current nursing concepts and priorities that focus on the humane face of care in the context of ever-increasing medical specialisation and technologies. ‘Care attitude’ might be considered to relate more to the emotional aspects and interpersonal dimensions of nursing and includes complex phenomena such as sympathy, empathy, compassion, kindness, maintaining dignity, bringing joy, and particular kinds of friendship or friendship human connection. For example, after numerous investigations, a patient affected by cancer must endure an arduous and specialised treatment; careful friendly explanation helps alleviate anxiety and adjust to care technology bearable [6]. These themes have global relevance and extend beyond nursing, with such references to the caring attitude observed across the Osler seminar series. For example, seminar speakers from Asia discuss the support of people living with residual disfigurement in Asia following burn surgery in China and alleviating the quality of life impacts of managing elephantiasis in India.
An investigation into the therapeutic effectiveness of nursing referred to in the Osler Nursing Seminar highlighted the significance of the interplay of expressive-personal dimensions of nursing care, integrated with the instrumental technical dimensions, and how both nurses and patients may construe these as having therapeutic significance and impact [ 7, 8]. Professor Steven Ersser’s ethnographic study highlighted the significance to patients of the ‘presentation of the nurse’, highlighting the significance of the interpersonal dimensions of nursing, such as the nurse’s comportment, including ‘being friendly’, their existential presence for patients’ at a time of suffering and the crucial anchoring nature of the nurse-patient relationships, and providing a foundation for technical and intimate physical care. The latter was identified as a distinctive case of helping or the therapeutic relationship created through the provision of nursing care.
In contemporary nursing, with the development of nurses interpersonal skills, there is a greater realisation of the central place of self-awareness to enable such relationships to be developed, and so the educational value of a habit of reflective practice and a heightened awareness of the importance of the nurses' wellbeing and protection against personal burnout [8, 9]. Furthermore, the development of the nursing curriculum for pre-registration nurses and new UK nursing standards explicit the centrality of ‘best practice communication skills and approaches for providing therapeutic interventions’. This is a skilled activity that can be cultivated through education [10].
The significance of care attitude has been accentuated of late through the impact of wearing protective clothing by nurses through the COVID-19 pandemic, in which interpersonal barriers can aggravate the isolation or loneliness of patients or residents in care homes, disrupting the subtle displays of friendliness and relating. Through the pandemic, social distancing and isolation within care contexts resonate with the experience over centuries for the management of those with leprosy, which was mostly managed by isolation. For nurses, making meaningful connections is a caring objective and a foundation of care. In caring for those with infectious diseases, social isolation is activated by fear or disgust, with protective clothing and equipment potentially impeding the building of therapeutic relationships. Yet subtle efforts have been made to aid communication and personalisation with staff writing their names on their clothing and using transparent face masks.
The concept of the care attitude in nursing may be construed as a spectrum of personal and value-based qualities, ranging from sympathy, compassion, empathy, and maintaining dignity and kindness. In Ersser’s study, the friendly demeanour of the nurse within the ward setting, such as verbal or non-verbal friendly acknowledgement of the patient and conveying their presence, was construed as therapeutic by patients through reducing social isolation, fear, and opening up communication opportunities [8]. Indeed, the social nature of nursing engendered a culture infused with banter, laughter within everyday social interaction, listening and expressive touch, and thereby conveying the nurses’ presence, helped to build relationships and trust and, in doing so, helped create a buffer against the stresses imposed by illness and treatment. Terence Ryan, following the lead given by [5], argued that friendship is a key dimension of the care attitude, with its various facets of compassion, including empathy and kindness. He argues that friendship, not simply compassion, should be further analysed as a component of ‘care technology’ curriculum, a skill and intervention required by both doctors and nurses, and one requiring performance and cultivation.
1.2. Care Technology
Care technology embraces the human exercise of technical skills that must be learned to practice clinically as, for example, from the simple low technological use of a bandage to the complexity present within high technological environments of Intensive Care or an operating theatre, where care is embraced despite a patient’s loss of consciousness. They are often dependent on employing complex tools developed from a scientific evidence base. The Osler seminar series embraced topics representing care technology, such as the contemporary management of burns in China. Here technological developments in wound healing have had to be accompanied by improved standards of nursing education to achieve significant progress in patient survival and quality of life, whether in a hospital or after discharge to a family or community often lacking in altruism; this was exemplified in the seminar by Prof Zhoafan Xia from Shanghai’s leading military burns hospital.
Another seminar focused on a single symptom and sign, the swollen limb, and this reflected the multidisciplinary nature of collaboration needed to tackle otherwise intractable health problems such as elephantiasis; but the need for active nursing contributions to improving the skin barrier and enhance the quality of life, with clinical research [11]. Other holistic models taking account of patient education and empowerment were illustrated, such as the therapeutic model developed at the South Indian Institute of Applied Dermatology, supported by the Bill and Melinda Gates Foundation. Nurses Professor Christine Moffatt and Dr Jill Brooks outlined nurse-led initiatives to support the frail elderly in the UK affected by immobility and sitting with their legs dependent, acquiring swelling from gravitational affects. Again, the nurses’ crucial interpersonal role in persuading the patient to move, elevate and exercise lymphoedematous in their ankles requires more than just compassion, but its integration with skilled education and support, demonstrated through clinical research in the UK, Uganda and Ethiopia, where the problem is widespread, leading to significant quality of life impacts [12, 13].
1.3. William Osler and Nursing
Osler is likely to have read the 1892 text, Nurses and Nursing, by the American nurse Lisbeth Price from Philadelphia [14], in which she advocated blending “the humane with scientific nursing”. Osler was frequently asked to address a nursing audience as he embraced and valued nursing, along with the range of health practitioners and other systems of health care.
He gave several recorded orations on nursing, which included excerpts from commentaries listed in Table 1.
Charles Bryan, in his Sir William Osler: an Encyclopaedia [15] writes that ‘’on balance Osler promoted the professionalisation of nursing, although his overall attitudes were characteristic of his time and place,” reflecting sometimes Osler’s chauvinism and less enlightened views than his nursing colleague, Mary Nutting (1858-1948), Head Nurse at Osler’s workplace, Johns Hopkins in Baltimore, who co-authored a four-volume History of Nursing (1907-1912) [16]. She graduated from the University’s first nurse training programme in 1891 and helped find a modern nursing programme at the school. In 1885, she reflected on what nurses should learn but requested progressively that ‘’the day (be) arranged for study, less work and more education”. Nutting went on to become a pioneer in the development of University education for nurses by contributing to the early development of university education opportunities for nurses at the influential Columbia University Teachers College, which became a significant base for the development of academic nursing leaders.
The section in the Encyclopaedia on William Osler on ‘Caring ‘describes its components as beneficence, empathy, sympathy, and compassion. Beneficence (“doing good”) is caring at its most fundamental level and a cornerstone of medical ethics. Empathy (“in feeling”) requires, at least intellectually, understanding how the patient feels. Osler was unequivocal, recognising the imperative of putting yourself in the patient’s place and mental state. Sympathy (“like or fellow feeling”) stipulates an emotional response by the caregiver to another’s distress. It can lead to burnout, and repetitive sympathetic responses can dull its effect. Compassion (“suffering with”) literally means to take on another’s burden. Osler was a great admirer of the 17th-century physician Sir Thomas Browne who wrote; “For compassion we make another‘s misery our own” [17]. Furthermore, Charles Bryan, in his Sir William Osler: an Encyclopaedia, reflects Osler’s thinking that “compassion is best seen as an action, not as an expressed feeling” [15].
At the time of Osler, the UK Minister of Health, Arthur MacNalty, wrote [18] that he advanced the science of medicine, enriched literature, and the humanities, yet individually he had greater power. This greater power, he reports, was his capacity for friendship. Osler repeatedly describes the importance of cheer and friendliness. He attributed such emphasis during thousands of years of practice to Confucius, Hippocrates, Galen, Burton, Browne, and others; thus, in Burton’s Anatomy of Melancholy [19], one reads, “Find a friend who makes you laugh”. Interestingly, the research investigated how patients construe and experience the therapeutic effect of nursing; this dimension of the nurse's behaviour captured the concept of the ‘presentation of the nurse,’ gathering data from patients and nurses that referred to the significant nature of nursing interaction, not just in terms what is undertaken as technical actions, but specifically how these are delivered through the nurses' comportment [8]. These were experienced by patients not only as satisfying but therapeutic in effect; that is, they were linked to tangible outcomes for them, such as their willingness to disclose personal concerns or convey their lack of understanding to self-manage, and in doing so provided a basis for their nursing needs to be met. Osler highlighted dimensions of the health professional’s comportment, such as the role of cheer, and advised that “It is an unpardonable mistake to go about among patients with a long face [20]”.
| 1904:(Osler, 1904) |
|---|
| There is no higher mission in life |
| The trained nurse has become one of the greatest blessings of humanity, taking place beside the physician and the priest and not inferior to either. |
| 1913:(Osler, 1913) |
| Nurses have seven virtues: tact, tidiness, taciturnity, sympathy, gentleness, cheerfulness. |
| A more comprehensive education and training would elevate nursing to the rank of scientific art like our own and would secure to its members the social position and material rewards that belong and are generally given to those who combine a scientific education with a useful calling.” |
The Oxford Centenary Seminars highlighted the importance of the care attitude to Osler, and the integration of both caring and science, across the spectrum of topics. The first seminar focused on the role of the attitude of care amongst Asian Children. Arising out of the observation of animal cruelty in China, through the fur and food industries, the charitable organisation ACTAsia was launched 12 years ago (www.actasia.org) to alleviate the suffering of animals. ACTAsia developed a successful curriculum in primary schools to promote the care for animals by children; it has become one of the most successful charities in China, contributing to promoting public support in China to reduce caging of wild animals and viral spread from animals to humans. Terence Ryan thought it beneficial to forge a link here that remembered Osler. ACTAsia's Caring for Life Education (CFL) programme, which provides a digital platform for university initiatives and industry, was launched from the Oxford seminar. CFL was developed from UNESCO’s Four Pillars of Education and is a foundation course in the Learning to Live Together Programme, promoting compassion and kindness in Asian societies and enabling children to develop emotional intelligence, to benefit not only animals but also the environment, the frail disabled or disfigured. The same theme has been taken up and amplified by Join Hands in Caring for life seminars and webinars in Pakistan (www.joinhands.org).
1.4. Green Templeton College, Oxford School Of Nursing and Midwifery and Nursing Development
For over forty years, Green Templeton College, Oxford (originally Green College), has actively promoted the discussion of the role of all health professions. This included correspondence in 1990 from the Office of the Vice Warden, Dr.Terence Ryan, when he and the radiologist Dr. Basil Shepstone sought to assist nursing colleagues in pursuing eligibility for postgraduate studies in nursing at the University of Oxford. As Green College came on the scene, a firmer partnership between doctors and nurses was discussed, and this continued to be expressed by the management influence of Nigel Crisp at the John Radcliffe Hospital, Oxford. The intention of establishing nursing as a clinical-academic discipline in Oxford was achieved in 1992 when Oxford Brookes University developed and offered the country’s second MSc in Advanced Clinical Practice and an undergraduate degree nursing programme. Oxford sought to attract graduate nurses and became increasingly involved in a range of nursing practice and research developments, including care of people following treatment for breast cancer, leg ulcer research, and community diabetes control. Links between Green Templeton College and nursing in Oxford were consolidated when in 1989, Dr. Susan Pembrey established the Institute of Nursing in Oxford to promote innovation and the rigorous evaluation of practice [21]. She also forged alliances with both universities in Oxford, University of Oxford, and Oxford Brookes University, to promote research and development in nursing, with clinically-based developments in nursing areas such as older person’s care, acute nursing, and dermatological care. Dr. Pembrey and the Director of Research, Dr. Alison Kitson, both within links to Green College, recognised and promoted work on the therapeutic nature of interpersonal relationships in nursing’s clinical effectiveness, including supporting the doctoral work of Steven Ersser in this area [7].
Lord Crisp has gone on to be a major advocate for the international Nursing Now movement, highlighting the critical role that nurses play in effective and sustainable health systems [22]. Nursing Now seeks to empower nurses to take their place at the heart of tackling 21st Century health challenges and works in collaboration with the World Health Organization and International Council of Nurses.
In a 1985 Annual Green College, Oxford lecture, the Professor of Nursing at the University of Manchester, and later patron of the Oxford Institute of Nursing, Baroness McFarlane of Llandaff, stated in a presentation on nursing education that “Care is often physically orientated and lacks provision for psychological, social, and spiritual needs”; during training, skills in empathic relationships are not improved. Indeed, she then argued that nursing education appears to inhibit rather than foster human relationships” [23]. She went on to warn that “If we do maintain the present position, then we must absolve nurses from striving to meet unattainable expectations. Consumers of health services must be made aware that they cannot expect a nurse to be caring; she will give maintenance care, and in some roles custodial or routinised care, but she will not be equipped to think, make decisions, or recognise changes, still less to comfort, console, counsel, or teach”. Baroness McFarlane and the Manchester nursing group were early pioneers in the development of University education for nurses in the UK in the nineteen sixties. This reflected the need to reconcile the interpersonal and technical dimensions of care and the need for education to effectively integrate these aspects.
1.5. Some Contemporary Perspectives on Nursing Over 50 Years
When Dr. June Clark (1986) referred to seven reports on UK nursing education over 50 years, none of which were fully implemented, she quoted Oscar Wilde and said expecting too much would be a “triumph of optimism over experience” [24]. In the British Medical Journal, there were articles jointly by medical and nursing editors [25] questioning who was at fault, medicine failing to share or nurses failing to take responsibility. When Clark wrote Nursing: an Intellectual Activity [26], there were many, from both professions, who were repelled by talk they regarded as jargon such as phrases of “coherent and holistic care” and “extant definitions of quality care”, however, Clark highlighted the importance of nurses taking responsibility linked to the requirement to undertake a robust university education. All this was debated as a national issue, but those who worked in resource-poor regions of the world, such as much of Africa, conveyed that nurses were operating worldwide with high levels of responsibility, playing the role of family practitioner, social worker, hospital doctor or administrator [27] and promoting access to health care at scale [28].
Project 2000, a key reform for UK nursing education, was implemented in 1990, replacing the apprenticeship system, in which nurses were trained in hospitals and treated as workers, with an educational reform in which nursing education was transferred to British universities, securing their status as supernumerary undergraduate students [29]. The issue of whether compassion was learned or lost as an apprentice or as a learner at university continued to be debated [30], especially when there was media attention drawn to lack of care in hospitals or care homes. More recently, Dr. Ann Bradshaw, a former nursing academic at Oxford Brookes University [31], discussed the Mid -Staffordshire inquiry by Robert Francis QC, arguing that degree level nursing may have been at the expense of experience of the basic tasks that all nurses should be able and willing to do. Bradshaw focussed on the restoration of compassion and competence through apprenticeship. However, The Royal College of Nursing’s Willis Commission [32] highlighted that there was no evidence that a university education undermined nurses’ ability to exercise the qualities of care and compassion and that, while some nursing care and responsibility are now delegated to health care assistants, registered nurses remained accountable in overseeing nursing teams.
Contemporary reflections on nursing, within the Osler context, were examined within the Oxford Osler Seminar by Kathleen Galvin, Professor of Nursing Practice at the University of Brighton [33], whose paper explored the importance of the philosophical life world view built on foundational human values, (humanised care) to support nursing’s interpretation of many dimensions of wellbeing and their centrality to nursing practice. She employed the term ‘caring science ‘as a distinct focus from biomedical science, following Scandinavian ideas. Her views are based on what is termed ‘life world’, drawing on philosophical literature which reflects the totality of how we experience ‘everydayness’, the seamless flow of the experiences and is inclusive of the whole range of human experience: how we experience time, space, being with others, mood and our ‘embodied sense or living, as this body’ or silence or awareness of our body. The seamless experience of these constituents is manifest as our life world.
Patients commonly experience life world disruptions such as 'falling ill,' embodied changes that a person must live with that are often very difficult to embrace, as well as being cared for in contexts where death is sometimes always close, such as in intensive care. With life world disruptions, the experiences of time, space, being with others, mood and embodiment can be radically altered. She gives an example of the importance of nurses being attuned to and responding to the depth and details of patient experiences, including unconsciousness to consciousness experiences. For example, by a ventilated patient, a context currently brought to the public’s attention through the COVID-19 pandemic. In addition, these fundamental ideas using life world as a foundation can illuminate new insights into human dimensions important in care and offer new ways of thinking about wellbeing [34, 35]. However, they also support the idea of the human face of care, its interpersonal dimensions, and practical steps taken to humanise care. This development can guide how a friendly, caring stance can be applied and be sustained in a busy practice. This has congruence with the earlier discussion on friendship being construed as a particular kind of care attitude, as characterised by Osler.
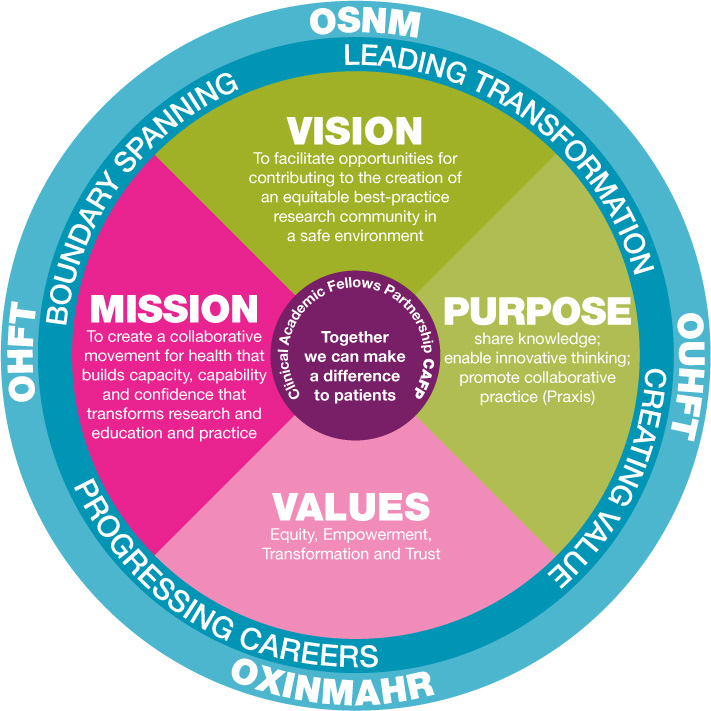
In another paper within the Osler Nursing Seminar, Dr. Mary Malone, Director of the Oxford School of Nursing and Sally Markwell Senior Lecturer in Public Health and Nursing, both from Oxford Brookes University, described the re-established Oxford School of Nursing and Midwifery (OSNM) as a partnership between Oxford University Hospital Foundation Trust, Oxford Health Foundation Trust and overseen by the Oxford Academic Health Partners. This initiative seeks to expand McFarlane's thinking in order to establish the decisive nurse capable of not only providing the solace of therapeutic friendship, which Osler valued so highly but also of conceptualising why and how this makes a difference in patient care. They described their work between 2018 and 2020 in developing, nurturing, and sustaining nurses who have both clinical and academic components to their role. Drawing on Parse’s philosophy of co-existence and the importance of ‘living rhythms’ [36], they suggested a modern Oxford model of clinical academic partnership in nursing, identifying the aspirations, motivations, and organisational components that make this work (Fig. 1).
According to Dr. Theresa Shaw, former Chief Executive of the Foundation of Nursing Studies, Osler seminar contribution continued with the theme of the central importance of nursing leadership and practice development to deliver on nursing reform, highlighting key developmental work undertaken in Oxford [37-41], which was built on by the Foundation, through its work with nurses and nurse-led teams for over thirty years across the UK.
Sharing her perspectives on the evolution of practice development, Theresa highlighted ways in which it remains important for a contemporary practice where nursing staff can be found in despair and at times brought to tears by cultures that focus on blame rather than learning; their wellbeing being compromised by an emphasis on efficiency over the quality of care practices.
Practice development and its emphasis on more facilitative and collective leadership forms have long been recognised as an approach to enabling the transformation of care practices [42]. However, more significantly, it can enable the creation of person-centred workplace cultures where staff feel valued and supported to give their best and where those experiencing care services feel cared for and safe [43]. She also drew attention to the central importance of nursing education in helping students develop their understanding of the principles of person-centredness and becoming attuned to their values and impact. Now, as people and services adapt to the consequences of the pandemic, it is even more the case that person-centredness and staff wellbeing must be a central theme through nursing curricula, key areas of research and development in nursing, and service and workforce planning.
Throughout the seminars, all speakers illustrated and described both dimensions of care technology and care attitude as becoming increasingly complex and contributing to an already overloaded pre-registration undergraduate nursing curriculum. Both dimensions have required educational development for nurses to fulfill not only core elements of the role of the registered nurses but also complex specialist and advanced practice roles, where nurses may provide nurse-led clinics and lead clinical services. Clinical nurse specialist roles are expanding, with an increasing number of nurses specialising in a variety of clinical fields, such as diabetes, stoma care, or wound healing, promoting access to health care, and where there was a clear need for high quality research evidence to underpin knowledge on how to improve the safety and effectiveness of practise. The thirty years of universal university education for nurses in the UK, and longer in the USA, has provided opportunities for nurses to develop the knowledge, both within and beyond the boundaries of each medical speciality. Inevitably, this has led to initiatives in multidisciplinary education, and it is becoming normative for nurses to play a leading part and at times forge multidisciplinary research teams. Some thought that nurses were required to join with medical students in their first years in a stem curriculum; for example, The Stem Doctor by Dr Anthony Chant was especially influential [44]. Interprofessional educational development continues across the UK with many nursing and health science centres.
The debate about the education and role of nurses is currently reduplicated in the debate about the need for and the type of nursing roles to promote access to health care in resource-poor regions, including the related but distinct generic role of the Community Health Worker (CHW) [45]. There have been recent international debates as to whether, in the resource-poor world, CHWs should be greatly expanded to meet the nursing needs of primary care [46]. According to the WHO, there is now a global community with more than 19,000 members in 177 countries, interacting on six global forums in four languages, which throughout 2019, debated the value of CHWs. The evidence is overwhelming that professionalized CHWs can greatly improve health delivery at low cost in countries at all income levels and are therefore vital to realizing The Universal Health sustainable target of Sustainable Development Goal 3, which aims to ensure the promotion of healthy lives and wellbeing for all at all ages. The range of demands is huge, and the curriculum for training is easily overloaded in prominent specialist areas such as midwifery or mental health. In the relief of the common harm of isolation in the resource-poor world, CHWs now play a major part. Specialities where there has been a shortage of medical specialists, such as dermatology, have seen the development of services in the UK in which clinical nurse specialists and advanced practice nurses have played a key role within multidisciplinary teams. However, nursing practice has often provided valued-added elements, such as the support and education needed to enhance treatment adherence, as a major element to enhancing treatment effectiveness, especially for the significant numbers of the global population living with significant long-term health challenges, where medicine's effectiveness is limited.
1.6. The Case of Dermatological Nursing
Professor Terence Ryan, custodian of the Osler's archives but also Emeritus Professor of Dermatology at Oxford, has led this series, and it seemed fitting to briefly examine nursing development from the perspective of a clinical speciality, as a bridge with medicine. Nursing development in Oxford has an established history, and these can be illustrated with the link to the clinical speciality, albeit one dimension. Nursing development within these specialties continues to improve access to health care, including not just medicine but also other aspects needed to adapt to health challenges, such as nurses promoting self-management strategies for those living with long-term health challenges.
During the evolving debate on the role of nursing, the Department of Dermatology in Oxford was willing to explore the division of labour between medicine and nursing and helped to facilitate reform of some of the medical/surgical roles to nurses and through its work with the Institute of Nursing in Oxford, led by nursing and practice development pioneer, Dr. Susan Pembrey (21). This provided a base for nursing research and development with practice-based Clinical Fellows linked to the Institute. The Department, through the work of Terence Ryan, Steven Ersser (Clinical Lecturer and Senior Nurse), and nurse Rebecca Penzer, went on to provide an international lead to nursing development promoting this debate in the dermatology field at the global level by setting up the International SkinCare Nursing Group, which later became affiliated with the International Council of Nursing. This Group was not afraid to provide leadership roles in health care and highlighted the potential of nursing to play an expanded role in promoting access to dermatological services worldwide that could not be adequately met by medicine [28]. The first service support provided was for the islands off the west coast of Africa to manage elephantiasis due to filariasis.
Nurse-led clinics promote access to dermatology care and wellbeing, supporting those who live with long-term conditions and offering effective self-management and patient education. Some of this work has extended into the traditional medical and surgical domain, such as nurse-led surgery, or has built on those areas in which nurses have established expertise, such as pinch grafting as a wound healing skill for leg ulcers. Prescribing for outpatients by appropriately trained nursing staff in a dermatology department is a safe and effective development [47] and has since expanded significantly. Nurse prescribing is now well established in the UK and in many health systems, promoting access to health care and providing additional support for treatment adherence through patient education and support.
The Oxford Department of Dermatology worked with the Institute of Nursing to support systematic practice development and the engagement of nurses in research alongside clinical practice, focused on key services such as the care of older people (McCormack), surgical care (Binnie), and indeed dermatology, through the evolution of lecturer-practitioner and other key leadership roles. The Department also worked with the International Committee of Dermatology to support several attempts in the resource-poor world to improve knowledge of skincare. In Guatemala, for example, this was opposed by dermatologists for fear of the loss of private patients [48]. However, adding some knowledge of skin conditions to nursing practice by providing weekend teaching sessions to 250 rural nurses significantly increased referrals to dermatologists in the capital [48]. This advanced the argument for the need for a care delivery model that offers basic skincare at a primary care level supplied through the nursing service while drawing on specialists (medical and nursing) who are often based in secondary health care services [49].
1.7. Changing and Evolving Professionals’ Boundaries and Health Care Systems
A systematic review of 11 trials and 23 observational studies comparing nurse practitioners and doctors found that nurses had higher patient satisfaction and little or little difference in health status outcomes. Nurse Practitioners often had longer consultations, and no differences were found in prescriptions. In surgery, there were many jobs welcomed by the surgeon, such as assisting in theatre or post-operative nursing. The need to recruit nurses was always balanced by the need to keep them in the job. Dissatisfaction with roles, poor salaries, and early retirement within a year of qualification or not even completing training has often been an enduring source of concern. The Project 2000 educational initiative aims to have all care in the U.k. given by university-educated nurses rather than student nurses who serve as workers while still in school. The development of University schools of nursing has driven a commitment to advance the evidence base of nursing as a global initiative, stimulating both empirical research and the utilisation of research findings, which was built on foundations set by a later Oxford Professor of Medicine, David Sackett [50]. Some nursing practice research units that were initially focused on pressure ulcers, urinary tract infections, and nutrition were cautioned not to lose contact with the medical profession. However, widespread research practice linked to the NHS through the National Institutes for Health Research, and the National Institutes for Health in the USA, now actively promotes high standards of interdisciplinary research and development, educating and developing nurse scientists alongside other clinicians, with research in several areas being led by nurses, including those in formal clinical-academic roles.
CONCLUSION
Aside from the 100th anniversary of Osler's death, it was also the 100th anniversary of the Nurses Registration Act, which set educational standards for nursing and introduced regulation of the profession. Nursing is the largest health profession in the world. Nurses and midwives account for nearly 50% of the global health workforce. There are now 27.9 million nurses, of which 19.3 million are professional nurses, and 2 million midwives make up half of the global health workforce. The medical journal “the Lancet” foresaw a future in which the full potential of ‘Nursing’ is better realized; but they emphasised the adverse impact of gender biases and shortage in Africa, Southeast Asia, and the Eastern Mediterranean [51]. The current State of the World’s Nursing 2020 report highlighted that the world does not have a global nursing workforce commensurate with the universal health coverage and UN Sustainable Development Goal targets. Furthermore, over 80% of the world’s nurses are to be found in countries that account for half of the world’s population [52].
Much has been achieved across health systems worldwide to develop and provide care technology, but not enough is done to ensure that it is suitably counterbalanced by developments in education, research, and practice that support the concomitant development of care attitude and its therapeutic impact. Engaging in the writings of Sir William Osler and reflecting on how to enhance the therapeutic power of friendship and support provided by nurses in all health systems, including the care provided by the Community Health worker, reveals the benefits of such ‘therapy’, whether in sophisticated health systems, but especially in resource-poor regions of the world. Nursing is a cost-effective use and investment in fundamental health care. Yet, in many countries, the nursing service remains a poorly recognised and neglected resource. A testament to the central importance of the nursing service worldwide is the prominent recognition given to nursing by the World Health Organisation (WHO) in 2020 (and now extended to 2021) through the WHO International Year of the Nurse and Midwife.’ This demonstrates the significant role that nursing services play worldwide, across all health systems, and not least, as shown by its most exceptional contemporary test, its fundamental response to the 2020-2021 global COVID-19 pandemic.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Not applicable.
AVAILABILITY OF DATA AND MATERIALS
Not applicable.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


